AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
Paroxysmal nocturnal dyspnea11/30/2022  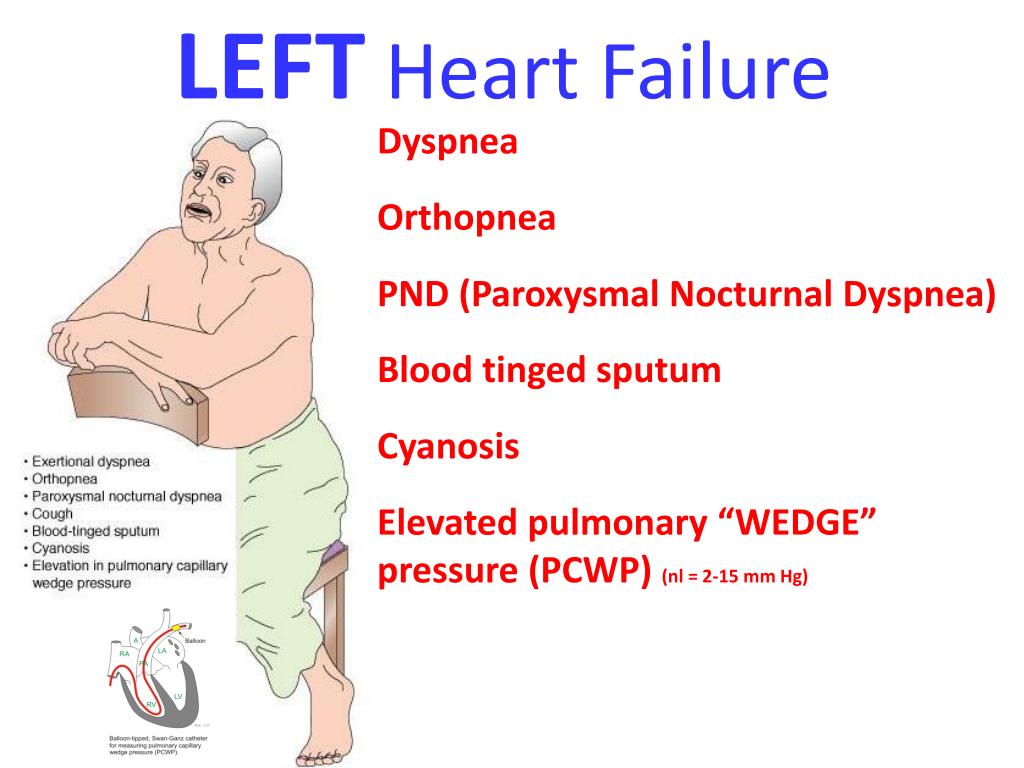
The symptoms of PNH occur because of the production of defective blood cells and because the bone marrow does not produce enough blood cells. The specific symptoms of PNH vary greatly from one person to another and affected individuals usually do not exhibit all of the symptoms associated with the disorder. Severe bone marrow dysfunction results in low levels of red and white blood cells and platelets (pancytopenia). Affected individuals also have some degree of underlying bone marrow dysfunction. In addition to hemolysis, individuals with PNH are also susceptible to developing repeated, potentially life-threatening blood clots (thromboses). Hemoglobin in the urine may not always be visible to the eye. However, hemolysis in individuals with PNH is a constant process (i.e., it does not occur only at night). 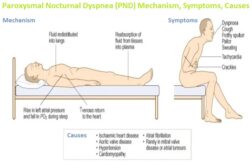
This finding is most prominent in the morning, after the urine has concentrated overnight during sleep. Individuals with hemoglobinuria may exhibit dark-colored or blood colored urine. Hemoglobin is the red, iron-rich, oxygen-containing pigment of the blood. The destruction of red blood cells (hemolysis) by complement leads to episodes of hemoglobin in the urine (hemoglobinuria). These defective red blood cells of PNH are extremely susceptible to premature destruction by a particular part of a person’s own immune system called the complement system. Some hematopoietic stem cells in individuals with PNH are defective and consequently produce defective blood cells. These cells grow and eventually develop into red blood cells, white blood cells and platelets. Hematopoietic stem cells are created in the bone marrow, the spongy center of the long bones of the body. It is an acquired hematopoietic stem cell disorder. Paroxysmal nocturnal hemoglobinuria (PNH) is a rare disorder in which red blood cells break apart prematurely. 5 Myths About Orphan Drugs and the Orphan Drug Act.Information on Clinical Trials and Research Studies.Monitoring posture in future devices may provide valuable insight for the remote management of heart failure patients. Night-time elevation angle is indicative of these symptoms, presumably reflecting the tendency of patients to sleep partially elevated to avoid dyspnea. 
Conclusion: Orthopnea & PND are key symptoms of heart failure. Selecting an NTEA threshold of 14.8 0 yielded a sensitivity of 83% and specificity of 76%. A receiver operating characteristic (ROC) curve analysis (see figure) yielded an area under the curve of 0.79 for NTEA detecting O-PND. Results: Patient visits associated with O-PND (n = 24) had an average NTEA of 23.2 ± 2.8 0 (mean±standard error), compared to an average NTEA of 10.7 ± 1.7 0 for those patient visits not associated with O-PND (n = 41, P = .0001 using non-paired t-test). We compared the device-determined night-time elevation angle (NTEA) for patient visits with and without reported O-PND symptoms. At each patient visit, O-PND symptoms were assessed. Methods: 46 HF patients (35 male, 45–83 years of age, NYHA class I-III) in the MultiSENSE study wore an external posture monitoring device for a few days (0.9–14) at a time. We evaluated the use of automated posture sensing in assessing O-PND in HF patients. These postural symptoms are typically assessed by asking about patients' sleep angle in terms of number of pillows. Guidelines for HF patient management recommend routine assessment of O-PND. Background: Orthopnea and paroxysmal nocturnal dyspnea (O-PND) are cardinal signs of worsening heart failure (HF). 
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
